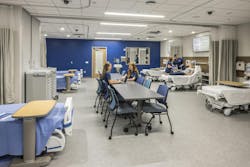
A building boom is underway in higher education to remedy a continuing nursing shortage.
Many colleges and universities are constructing new facilities, renovating existing nursing schools and other medical training space or are planning to do so. According to Becker’s Healthcare, more than 130 new nursing school construction projects and programs started in 2022.
Expanding nursing school capacity has accelerated in recent years because of an exodus of nurses from the profession. A massive wave of departures has been attributed to the pandemic. A National Council of State Boards of Nursing study said an estimated 100,000 nurses quit their jobs amid the global health crisis, and an additional 600,000 nurses plan to leave by 2027.
By creating additional space for nursing education, colleges and universities can expand their capacity to enroll qualified applicants. Adding space also addresses the need for nursing schools to modernize their facilities to meet the training requirements of an evolving and complex health care environment.
Patient Simulation Centers
A sizeable number of these facility upgrades are patient simulation centers. Accreditation requirements and competition among nursing schools to attract the best students spur increased demand for simulation spaces.
Examples include the University of South Florida Health College of Nursing expansion in Tampa, which is adding space for a patient simulation program and clinical care training. Another is a 16,000-square-foot renovation at Georgia State University’s Lewis College of Nursing and Health Professionals in Atlanta. The improvements include simulation space, clinical skills labs, and offices.
Also in Georgia, Emory University’s Nell Hodgson Woodruff School of Nursing has benefited from the new Emory Nursing Learning Center (ENLC), a 70,000-square-foot, $20 million patient simulation and professional development facility.
Since the ENLC’s completion in September 2022, the Emory School of Nursing has been ranked as the No. 1 program among graduate nursing schools. The new facility offers a transformative nursing student experience, blending a modern and aesthetically striking design with Emory’s celebrated past.
Health care simulation facilities have traditionally integrated with nursing schools situated on primary campuses. However, the ENLC and other nursing school simulation facilities operate at off-campus sites. Some schools have repurposed underutilized off-campus buildings to house simulation centers when on-campus space is hard to find.
Moving to a New Community
For Emory, an adaptive reuse project was the best approach for its simulation center. The ENLC occupies a 60-year-old former bank building in downtown Decatur, where students learn to care for patients in hospital, clinic, and home apartment settings. The facility also provides continuing education to nurses.
Emory wanted to consolidate its simulation programs under one roof, and because of space constraints, the only way to accomplish this was going off campus. They chose Decatur because of its public transport connectivity and its proximity to Emory’s Atlanta campus and local healthcare providers. This location improved interaction between Emory nursing students and Emory Healthcare nurses, which will help develop students’ skills and practice procedures.
Converting the mid-century office building into the simulation facility is also expected to revitalize the nursing school’s brand and increase diversity in student enrollment. Another benefit is that the Decatur facility is within walking distance of restaurants, hotels, and shops and offers public transportation to shuttle students to and from the Emory campus.
The renovation redesigned the building’s first four floors and basement and added modern simulation spaces that replicate examination and operating rooms, labor and delivery, home health, and telemedicine scenarios. The facility also has classrooms, supporting educational spaces, a student commons area, a digital media studio, a lobby, and offices. Plans call for adding space where students can practice with a heart-lung machine.
The ENLC’s design uses best planning practices such as placing briefing rooms near the simulation areas, standardized patient prep rooms, and spaces built to ensure maximum privacy and superior acoustics.
Design Challenges
Patient simulation spaces are more complex to design and build than college classrooms or labs.
Designing the ENLC required creating space for advanced medical technology to train students in the latest care delivery practices. For example, audio-visual systems designed for the facility’s high-fidelity simulation spaces were installed to replicate medical procedures in mock patient rooms.
The A/V technology requires a network isolated from the university’s system to capture and transfer patient data. The data goes to a central system, or “brain,” where faculty and students can review it. The project also required medical gases to be piped into patient headwalls.
For most situations, compressed air and vacuum are sufficient for simulation, but occasionally, actual medical gases are required. In the operating room, oxygen is piped into the headwalls for ventilators because compressed gas wouldn’t work correctly with these machines. Training headwalls with built-in compressors is an option when plumbed medical gas is cost-prohibitive, but the noise they create can be distracting when trying to simulate an authentic healthcare experience.
Nursing schools upgrading their facilities should seek professionals with medical design experience, specifically patient simulation facilities and higher-ed building projects. Medical equipment planners are also integral to the success of these projects. They are responsible for specifying, procuring, and coordinating the medical equipment involved in these projects and coordinating utilities such as power, technology, plumbing, and medical gases.
During the pandemic, supply-chain bottlenecks, virtual meetings instead of in-person discussions, and other Covid-related challenges disrupted building projects across the country. Regular collaborating and communicating throughout the process will help keep a project on track.
Finding Funding
Creating simulation facilities can cost millions of dollars, a steep financial barrier for many nursing schools can’t overcome without help.
Fortunately, governmental entities and philanthropic organizations have recognized the critical need for these facilities and have made sizeable contributions to cover some of the cost of nursing building projects and training programs. At the ENLC, a fundraising program was launched to help with the building’s construction and operational costs.
However, schools with limited financial resources can still find innovative ways to expand nursing education programs until more funding becomes available.
For instance, hospitals have provided space for nursing education. Before opening ENLC, one of the wings at Emory University Hospital, Wesley Woods, was used for the patient simulation program until the school’s enrollment outgrew that space. Baylor University also uses space at a Dallas hospital for the same purpose.
The continued strength of the nation’s health care system depends on a plentiful and reliable supply of nurses and other medical professionals to provide patient care – from the biggest cities to the smallest towns. New and planned nursing building projects and training programs are laying the groundwork to ensure the country continues to provide high-quality, safe health care delivery in the years ahead.
Graham Sinclair ([email protected]) is an associate principal and health practice leader at The Beck Group, an architecture and construction firm specializing in integrated design-build projects.
About the Author
Graham Sinclair
Graham Sinclair ([email protected]) is an associate principal and health practice leader at The Beck Group, an architecture and construction firm specializing in integrated design-build projects.